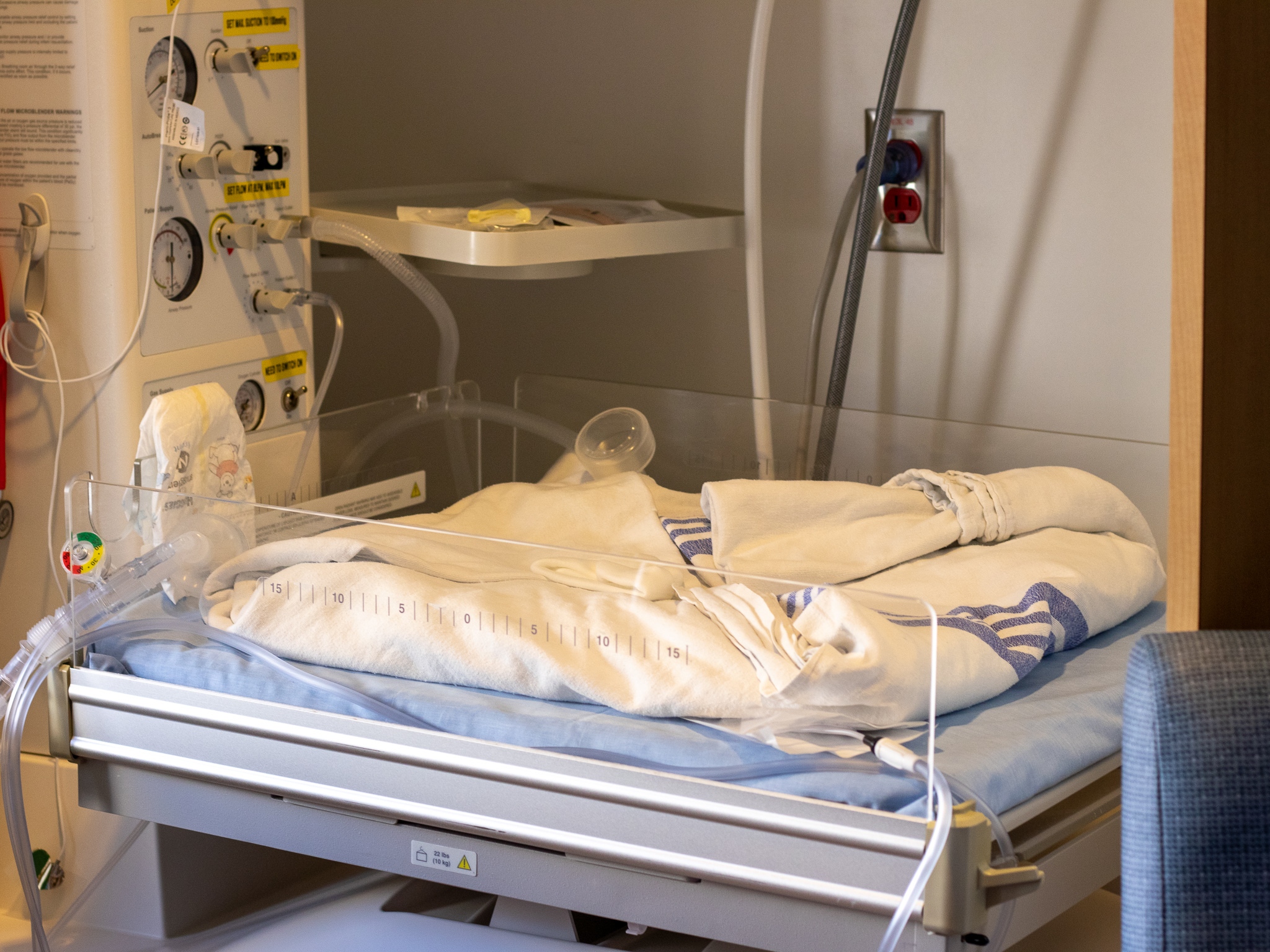
Medical Interventions
If you are pregnant, chances are good that you will deliver your baby vaginally, but there are times when a medical intervention (procedure) is needed for the safety of the birthing parent or baby. Even if you plan on having a vaginal birth, it's a good idea to know about them in case the unexpected occurs.
At times, medical interventions are offered to ensure you and your baby are safe and healthy during childbirth. Your health care provider will talk with you and your support person about options that are not part of routine care.
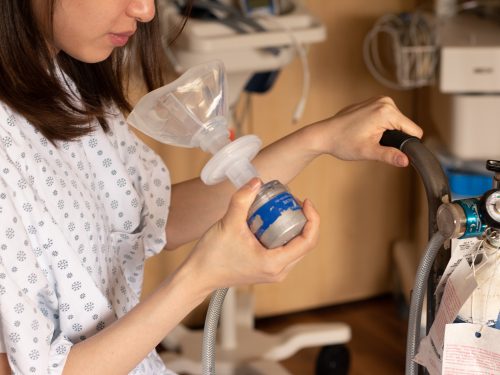
Assisted deliveries (use of a vacuum or forceps to help the baby come out) and Caesarean Sections are two common medical interventions that might be presented if deemed necessary by your maternity care provider.
What is a Caesarean Section?
A Caesarean Section (commonly referred to as a “C-Section”) is a surgery in which your baby is delivered through a cut in your belly and uterus. The majority of people having a C-Section will receive a regional anesthetic (either by an epidural or a spinal). In this case, you are awake during the surgery and birth but your pain is controlled. Your partner or support person can be in the operating room. You’ll likely be able to hold your baby skin-to-skin right after or soon after the birth. If you’re too sleepy or unable, your support person can hold the baby skin-to skin until you’re ready to do so. If you require a general anesthetic, you’ll be asleep during the surgery and birth and your partner will not be permitted in the operating room.
The need for delivery by C-section is based on the baby's and new parent’s wellbeing and medical conditions. In most cases, the birthing parent is awake during the birth but given very strong pain medications. Newborns can stay with their parents soon after birth for skin-to-skin in the operating room.
At the Birth Centre, we will make every effort to keep you and your family together during a C-section as well as afterwards during post-operative recovery. Birthing parents who are stable and did not receive a general anesthetic can complete their post-op recovery on the Birth Centre in their delivery room.
Depending on the reason for your first C-section and the type of incision that was made, you may be able to deliver your next baby vaginally. For more information, see Vaginal Birth After Caesarean (VBAC)
To learn more about Caesarean Section, click here.
What is an Assisted Delivery?
Medical assistance is offered if the labour becomes stalled during the pushing phase and/or if the baby has heart rate concerns and needs to be delivered quickly. This is usually done by application of a vacuum or forceps. At times, an incision to the base of the vagina (called an episiotomy) may be performed in addition to the vacuum or forceps.
- For a vacuum-assisted delivery, your physician will place a soft plastic cup on the baby's head and suction is used to help pull the baby out. The baby’s head must be very close to the outside of the vagina in order for a vacuum to be offered. The cup can leave a bruise and swelling, but this will fade a few days after birth. A vacuum is often offered if there is a prolonged pushing stage of labour, the birthing person is exhausted and unable to push effectively, and/or the fetal heart rate slows, showing signs of distress.
- For a forceps-assisted delivery, your physician will gently place two metal instruments around the baby's head to carefully guide the baby out. The baby’s head must be relatively close to the outside of the vagina. Forceps can leave temporary red marks or slight bruises on the baby's head and face. They are used if a birthing person has a prolonged pushing stage of labour, for exhaustion and ineffective pushing, signs of fetal distress, and/or the angle of the baby’s head needs to be changed slightly in order to give birth vaginally.
- An episiotomy may be offered with either a vacuum or a forceps delivery, which widens the perineum by an incision performed by the doctor or midwife. This helps deliver the baby's head more quickly if required, for instance, if there are signs of fetal distress.
A summary of this information is also available in the Medical Procedures to Help Labour and Birth chapter of your Baby’s Best Chance Handbook.
Skin to Skin: the "Golden Hour"
Once your baby is born, either by vaginal delivery or by caesarean section, it is encouraged to have your baby placed skin-to-skin with you. Skin-to-skin offers many benefits for both you and your baby, such as making sure your baby stays warm and promoting bonding, soothing, and breastfeeding. Click here for more information about the Golden Hour and how to position your baby safely during skin-to-skin.
It is encouraged to keep baby skin to skin with you for the first hour after birth or until completion of the first breastfeed. Skin-to-skin can be provided by your partner if you are unable, or do not wish to do so.
If your baby requires some assistance after birth, he or she will be
taken over to the infant warmer and assessed by the medical team. You
will be encouraged to resume skin-to-skin contact with your baby once he
or she is deemed stable.
Please note: this video provides general information for Richmond Hospital Birth Centre. Please contact Birth Centre staff for the most up-to-date details.
Breastfeeding / Chestfeeding

Breastfeeding / chestfeeding offers you and your baby a host of health benefits. Human milk provides complete infant nutrition for the first 6 months. It is recommended that parents offer exclusive human milk for the first six months of life, and continue offering for up to two years of age and beyond.
Your milk changes as your baby grows so that it always provides the right nutrition for their development. It is easy for babies to digest, promotes a healthy immune and digestive system, and helps to promote mental and emotional development.
Sudden Infant Death Syndrome (SIDS)
Babies who are fed human milk may have lower rates of Sudden Infant Death Syndrome (SIDS), infections (colds, pneumonia, ear and other infections), digestive issues (nausea, vomiting and diarrhea) and serious illnesses like diabetes and childhood leukemia. Breastfeeding / chestfeeding is also good for birthing persons to lower risks of diseases such as breast and ovarian cancers. It is also a very convenient and cost-effective way of feeding your baby.
Initiating breastfeeding / chestfeeding involves skills that must be learned by both you and your baby. Birth Centre staff are here to discuss your infant feeding goals and offer feeding support during your hospital stay.
Richmond Hospital NICU
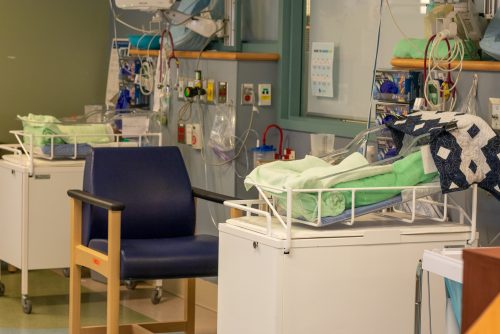
Richmond Hospital has a 6-bed Neonatal Intensive Care Unit (NICU) situated within the Birth Centre unit. Here, babies receive closer monitoring and specialized care by a team of specialty-trained NICU nurses and Pediatricians. Our NICU can provide care for babies born preterm at 32 weeks gestation or above. Babies born severely premature (< 32 weeks) or who require very extensive care after birth will need to be transferred to a different NICU facility.
If your baby requires admission to the NICU you and your partner will be able to see your baby and are encouraged participate in care at the discretion of the NICU staff. Skin-to-skin and breastfeeding / chestfeeding are supported, and feeding options will be explored.
A NICU admission package will be provided to you with guidelines and more information.
While your baby is in NICU, you and your family members may not be able to see and spend as much time with your newborn as you would like. To support family bonding as best as possible, and to provide you and your family members opportunity to see the baby even when away from the hospital, our NICU offers a live-streaming camera, free of charge. Please speak to your nurse to find out more.